Il est bien connu que le taux de testostérone totale diminue avec l’âge chez les hommes de 50 à 55 ans. de 0,8 à 1,61 TP1T/an, tandis que la testostérone libre commence à baisser à partir de 30-35 ans au rythme de 2 à 31 TP1T par an. À 70 ans, le niveau de testostérone d’un homme peut chuter jusqu’à 50 pour cent. Le problème de la baisse de la testostérone est l’un des plus urgents en médecine. Aujourd’hui, nous savons que les hommes entrent en andropause avec l’âge, comme c’est le cas pour la ménopause féminine.
Les raisons de ce déclin sont un dysfonctionnement de l’axe hypothalamus-hypophyso-testicules (HPTA), ainsi qu’une augmentation de la concentration de globuline liant les hormones sexuelles.
Auparavant, on pensait que le rôle de la testostérone n'était important que pour les caractéristiques sexuelles secondaires, la libido et la production de spermatozoïdes, mais il est désormais prouvé que cette hormone affecte presque tous les systèmes vitaux du corps. La testostérone agit sur le système génito-urinaire, le cerveau, les muscles, les os, le tissu adipeux et les cellules de la peau. On a récemment découvert que de faibles niveaux de testostérone augmentaient le risque de diabète. En outre, la testostérone est responsable de l’apport sanguin aux tissus, car de faibles niveaux de testostérone peuvent entraîner une altération de la circulation sanguine.
Signes cliniques de l'andropause
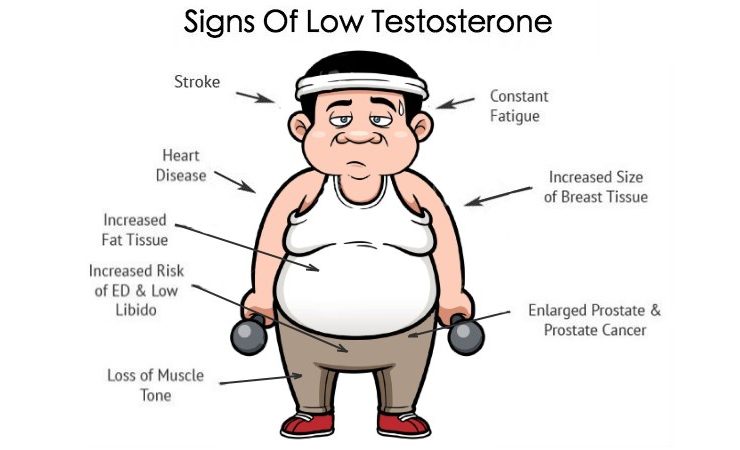
Une carence en testostérone entraîne des perturbations dans presque tous les systèmes et tissus. « la mémoire est altérée, la concentration de l'attention diminue, la vigilance mentale est perdue. Les yeux du patient semblent s'estomper, la tête et les épaules s'abaissent, les muscles deviennent plus lents, l'abdomen grossit, la poitrine ressemble davantage à celle d'une femme. En raison du faible taux de testostérone, les os deviennent fragiles et la peau s’amincit.
Les principaux signes et symptômes de l’andropause sont :
- Troubles génito-urinaires :
- diminution de la libido et dysfonction érectile
- diminution de la fertilité
- urination fréquente
- Troubles vasculaires :
- hyperémie soudaine du visage, du cou, du haut du corps
- les bouffées de chaleur
- fluctuations de la pression artérielle
- douleur au coeur
- vertiges
- se sentir essoufflé
- Les troubles mentaux:
- irritabilité accrue
- fatigue rapide
- affaiblissement de la mémoire et de l'attention
- insomnie
- états dépressifs
- diminution de l’état de santé général et des performances
- Troubles somatiques :
- diminution de la masse et de la force musculaire
- fragilité des os
- gynécomastie
- obésité
- calvitie
- amincissement de la peau
- diminution du niveau de testostérone totale et biodisponible
- augmentation des taux d'estradiol et de globuline liant les hormones sexuelles
- anémie
- augmentation du cholestérol
Âge de l'andropause
La probabilité d’apparition de l’andropause augmente avec l’âge.
Âge de l'andropause
- 40-49 ans 2-5%
- 50-59 ans 6-40%
- 60-69 ans 20-45%
- 70-79 ans 34-70%
- plus de 80 ans 90%
Effets secondaires des stéroïdes anabolisants chez les personnes âgées
Tumeurs
Pour les sportifs plus âgés, le risque d’hypertension, d’athérosclérose vasculaire, d’ischémie myocardique et de tumeurs malignes (prostate, glandes mammaires, intestins…) est bien plus élevé et augmente avec l’âge. Étant donné que les stéroïdes anabolisants augmentent le taux de division cellulaire, on pensait auparavant que ces médicaments pouvaient augmenter la fréquence des mutations. Si, chez les jeunes, le nombre de cellules mutantes est inférieur et que le système immunitaire est plus actif, le corps fait face à ce problème. Mais après 40 ans, le système immunitaire s'affaiblit, le nombre de cellules mutées commence à croître rapidement, ce qui peut entraîner l'apparition de tumeurs. Cependant, les données expérimentales modernes nient l'effet cancérigène des stéroïdes, à l'exception de la prostate et du foie (dans le cas de l'utilisation de médicaments hépatotoxiques 17-alkylés).
Gonflement et hypertrophie de la prostate
L'utilisation d'inhibiteurs de la 5-alpha-réductase est très efficace dans le traitement de l'hyperplasie bénigne de la prostate (HBP). À cet égard, des hypothèses ont été émises quant à l’effet négatif possible des androgènes exogènes sur la prostate. Dans le même temps, il a été constaté que ces maladies surviennent le plus souvent à un âge avancé, c'est-à-dire malgré la diminution des taux d'androgènes.
De nombreuses études moléculaires ont montré que le principal facteur pathogénétique dans le développement de l'HBP est une augmentation intracellulaire de l'activité de la 5-alpha-réductase, entraînant une augmentation du taux de 5-alpha-dihydrotestostérone dans les cellules de la prostate, et non une augmentation du taux de testostérone plasmatique. niveau.
Ainsi, l’HBP n’est pas considérée comme une contre-indication au traitement androgénique substitutif. De nombreuses études n’ont pas trouvé de corrélation entre les taux plasmatiques de testostérone et l’incidence du cancer de la prostate.
En présence d'hypertrophie prostatique, la testostérone est utilisée en association avec des inhibiteurs de la 5-alpha-réductase (Finastéride) comme traitement hormonal substitutif. Cela réduit quelque peu l'efficacité du cycle, mais réduit considérablement le développement d'effets secondaires androgènes, notamment sur la prostate. De plus, il est recommandé d'effectuer un examen préventif 2 fois par an, ainsi qu'une mesure en laboratoire de l'antigène spécifique de la prostate.
Alopécie (calvitie)
La perte de cheveux du cuir chevelu est également associée à une augmentation de la DHT, donc une thérapie combinée avec le Finastéride ou le Dutastéride peut prévenir efficacement la chute des cheveux.
Suppression de la sécrétion de testostérone
Comme vous le savez, grâce à l'utilisation d'androgènes, il est possible de supprimer la fonction endocrinienne des testicules et la spermatogenèse grâce au mécanisme de rétroaction négative. Cet effet est particulièrement visible lors de l'utilisation à long terme de stéroïdes anabolisants à des doses élevées.
Dans le même temps, la prise de 240 mg d'undécanoate de testostérone (ANDRIOL) pendant 6 mois ne s'est pas accompagnée d'une diminution du niveau normal initial de spermatogenèse. D'autres études n'ont pas non plus montré de suppression significative des taux normaux de gonadotrophines ou de testostérone endogène avec ce médicament, ce qui est probablement dû à la courte demi-vie de l'undécanoate de testostérone.
Ainsi, une thérapie post-cycle adéquate peut éliminer cette complication si l’andropause ne s’est pas encore produite. Après le début de l’andropause, un traitement hormonal continu est recommandé.
Atrophie testiculaire
En raison de la suppression de la sécrétion de gonadotrophines par le mécanisme de rétroaction, l'utilisation prolongée de stéroïdes anabolisants peut entraîner une atrophie et une désensibilisation des testicules. En d’autres termes, après l’arrêt de la testostérone exogène, les testicules ne retrouvent pas la capacité de sécréter leur propre testostérone. Par conséquent, les cycles longs doivent être accompagnés de gonadotrophine.
Érythrémie
La thérapie à la testostérone entraîne souvent une augmentation de l'hématocrite au-dessus des valeurs physiologiques en raison de la stimulation constante de l'érythropoïèse (associée à une production accrue d'érythropoïétine sous l'influence des androgènes). La plupart des auteurs recommandent de réduire la dose de stéroïdes lorsque les valeurs d'hématocrite sont supérieures à 51% et d'arrêter le médicament lorsque les valeurs sont supérieures à 54%.
Athérosclérose
L’effet des androgènes exogènes sur les taux de lipides sanguins est une question controversée. Traditionnellement, on pense que le risque accru d'athérosclérose et de maladie coronarienne chez les hommes par rapport aux femmes en âge de procréer est associé à un effet négatif des androgènes sur le profil lipidique. Cependant, plusieurs études ont montré que l'administration de testostérone entraîne une diminution des taux athérogènes de VLDL et de LDL, tandis que les taux de HDL anti-athérogènes restent relativement inchangés.
TRT pour les personnes âgées
Les principaux médicaments utilisés dans le traitement androgénique substitutif chez les hommes sont les esters de testostérone. Il existe des médicaments oraux, injectables et transdermiques. Actuellement, la testostérone alkylée en C17 (méthyltestostérone), qui a un effet toxique et cancérigène sur le foie lorsqu'elle est prise par voie orale, est pratiquement hors d'usage. L'hormone de croissance gagne en popularité, car elle est capable de rajeunir la peau et de renforcer les articulations et les ligaments.
Testostérone énanthate et Cypionate de testostérone sont la testostérone la plus courante aux États-Unis. Ainsi, un schéma posologique adéquat consiste en l'administration intramusculaire du médicament à la dose de 1 ml une fois toutes les 3 semaines. Souvent, une dose de remplacement est prescrite dans les 3 mois, suivie d'une annulation pouvant aller jusqu'à 3 mois.
Nouveaux médicaments
Les scientifiques sont constamment à la recherche de médicaments plus perfectionnés. Aujourd'hui, par exemple, le médicament injectable Nebido est apparu, qui doit être injecté quatre fois par an. Le médicament fournit une concentration stable de testostérone pendant trois mois : grâce à la libération progressive du « dépôt de pétrole ».
Testogels et les patchs de testostérone gagnent en popularité dans le monde entier, car ils doivent être appliqués sur la peau une fois par jour.
Relativement récemment, une nouvelle forme d’administration de testostérone a été créée : des comprimés sous la langue ou des plaques fixées aux gencives. Ces méthodes font l'objet d'essais cliniques.
 Maintain a Lean and Muscular Physique Staying relatively lean while having decent muscle mass is one of the best ways to support healthy testosterone levels. Excess body fat can increase estrogen and lower testosterone.
Maintain a Lean and Muscular Physique Staying relatively lean while having decent muscle mass is one of the best ways to support healthy testosterone levels. Excess body fat can increase estrogen and lower testosterone. Practice Power Postures Adopting confident “Superman” or power poses for a few minutes daily may help boost testosterone and reduce stress hormones.
Practice Power Postures Adopting confident “Superman” or power poses for a few minutes daily may help boost testosterone and reduce stress hormones.
 Eliminate Smoking and Limit Alcohol Quit smoking completely and reduce excessive alcohol consumption, as both can significantly suppress testosterone production.
Eliminate Smoking and Limit Alcohol Quit smoking completely and reduce excessive alcohol consumption, as both can significantly suppress testosterone production. Eat Enough Clean Calories Severe calorie restriction lowers testosterone. Consume sufficient high-quality calories from whole foods to fuel muscle growth and hormone production.
Eat Enough Clean Calories Severe calorie restriction lowers testosterone. Consume sufficient high-quality calories from whole foods to fuel muscle growth and hormone production.












